Introduction.
Antibiotics have been among the greatest medical discoveries in human history. Since the discovery of penicillin by Alexander Fleming in 1928, these drugs have saved countless lives by treating bacterial infections that were once deadly. However, this success has led to a silent and growing danger — antibiotic resistance. This global health threat occurs when bacteria evolve and become resistant to the drugs designed to kill them, making infections harder to treat.In Kenya and across the world, antibiotic resistance is spreading quietly but rapidly, fueled by overuse, misuse, and lack of awareness. The World Health Organization (WHO) warns that antibiotic resistance could cause more deaths annually than cancer by 2050 if urgent action is not taken. It is a threat that transcends health sectors affecting humans, animals, and even the environment.
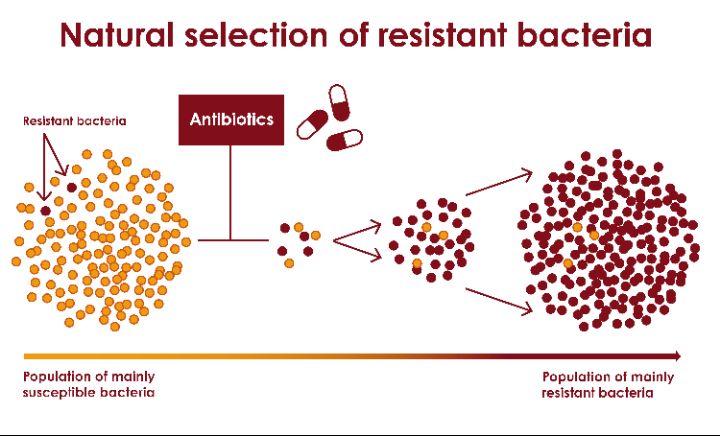
1. Understanding Antibiotic ResistanceAntibiotic resistance happens naturally over time, usually through genetic changes in bacteria. When antibiotics are used, they kill susceptible bacteria, but resistant ones survive and multiply. Over time, these resistant strains spread, making common infections difficult or impossible to treat.The problem worsens when antibiotics are misused such as taking them without prescription, using them for viral infections like flu, or not completing the full dose.
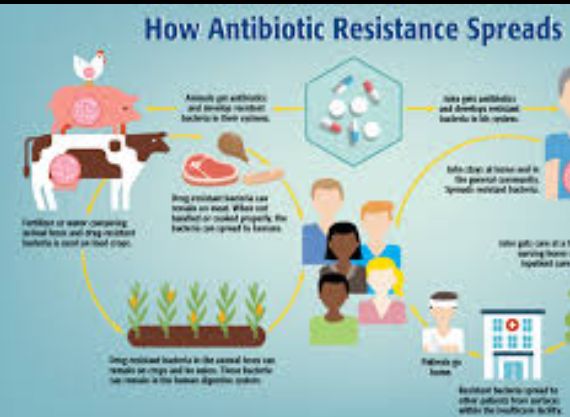
In Kenya, studies show that self-medication and easy access to antibiotics without prescriptions have accelerated the problem. Many people buy antibiotics from pharmacies without consulting a doctor, often using them incorrectly.Moreover, antibiotic misuse in livestock farming contributes to resistance. Farmers sometimes give antibiotics to animals to promote growth or prevent disease, even when not necessary. These drugs enter the food chain and environment, creating resistant bacteria that can infect humans.This complex web — involving humans, animals, and the environment — is known as the One Health approach, which recognizes that all three sectors are connected in the fight against antibiotic resistance.
2. The Global and Local Impact The effects of antibiotic resistance are already being felt worldwide. Common infections such as pneumonia, tuberculosis, urinary tract infections, and gonorrhea are becoming harder to treat because of resistance. Medical procedures like surgeries, cancer treatments, and childbirth also become riskier since patients rely on effective antibiotics to prevent infection.In Kenya, hospitals are facing increasing cases of antibiotic-resistant infections. For example, resistant strains of E. coli and Klebsiella pneumoniae have been reported in many health facilities. This makes routine treatments more expensive and less effective, especially for patients with limited resources.The economic burden is also severe.
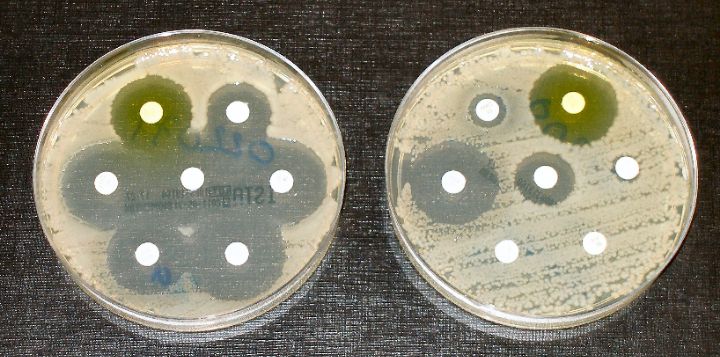
Longer hospital stays, more expensive drugs, and increased mortality put pressure on both families and the national health system. According to the Kenya National Action Plan on Antimicrobial Resistance (2017–2022), antibiotic resistance threatens to reverse decades of progress in healthcare and poverty reduction.Globally, WHO estimates that antimicrobial resistance could push up to 24 million people into extreme poverty by 2030 if unchecked. This silent crisis could therefore undo gains made toward achieving the Sustainable Development Goals (SDGs) particularly those related to health, hunger, and economic growth.
3. The Way Forward: Combating the Silent Threat To address antibiotic resistance, a coordinated global and local response is essential. In Kenya, the government has developed policies under the National Antimicrobial Stewardship Strategy, aiming to regulate antibiotic use in both human and animal health sectors. Hospitals are also encouraged to implement infection prevention and control programs, including hand hygiene, proper diagnosis, and rational prescribing.Public awareness remains a crucial part of the solution. People must understand that antibiotics are not a cure for every illness and should only be taken under medical supervision.
Completing prescribed doses and avoiding self-medication can help reduce the emergence of resistant bacteria.Healthcare professionals must also play their part by prescribing antibiotics only when necessary, and by educating patients about correct use. Laboratories and researchers should strengthen surveillance systems to monitor emerging resistant strains, ensuring timely action.The agricultural sector too must embrace responsible use of antibiotics in livestock production avoiding unnecessary use and improving animal hygiene.
At the community level, clean water, sanitation, and vaccination can prevent infections, reducing the need for antibiotics in the first place.Ultimately, fighting antibiotic resistance requires everyone’s participation from policymakers and doctors to farmers and the general public.
Conclusion.
The silent threat of antibiotic resistance is one of the most pressing health challenges of our time. It grows quietly but steadily, undermining our ability to treat infections and perform life-saving medical procedures. Without urgent action, even minor injuries or infections could once again become deadly.In Kenya and beyond, the battle against antibiotic resistance must be fought through awareness, responsible use, research, and strong public health systems. Antibiotics are a shared resource — once lost, they cannot easily be replaced. Protecting them today ensures that future generations will continue to benefit from their lifesaving power.The silence around antibiotic resistance must be broken — before it’s too late.—Would you like me to turn this article into a PDF with 4 animated photos included for presentation or submission?




